
Fractures of the wrist account for a third of all childhood fractures, with 1 in every 100 children presenting either a torus or a greenstick fracture.
Torus fractures are compression failures of the bone and are the most common fractures in children. [1] It is a common occurrence following a fall, as the wrist absorbs most of the impact and compresses the bony cortex on one side and remains intact on the other, creating a bulging effect. [2] For this reason, it is often referred to as an 'incomplete fracture' as the break is only on the one side. The compressive force is provided by the trabeculae and is longitudinal to the axis of the long bone [3]. The word "torus" originates from the Latin word "protuberance." [4]
Torus fractures are low risk and may cause acute pain. As the bone buckles (or crushes), instead of breaking, they are a stable injury as there is no displacement of the bone. [5] This mechanism is analogous to the crumple zones in cars. As with other fractures, the site of fracture may be tender to touch and cause a sharp pain if pressure is exerted on the injured area.
Physical activities or sports such as bike riding or climbing increase the associated risk for buckle fractures in the potential event of a collision or fall. As aforementioned, the most common buckle fracture is of the distal radius in the forearm, which typically originates from a Fall Onto an Outstretched Hand ( FOOSH) [6]. Such orthopaedic injuries are distinctive in children as their bones are softer and in a dynamic state of bone growth and development, with a higher collagen to bone ratio so incomplete fractures such as the buckle fracture are a more common occurrence. [7]
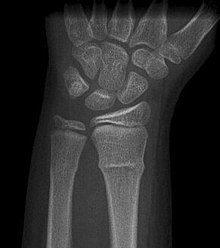
Buckle fracturs can be identified by performing a radiograph. The diagnosis of a torus fracture is made from both anterior/posterior and lateral projections. The typical features include:
- The buckling of cortical bone, which may appear as a small bulge or protuberance in the radius or ulna.
- The bone may have a slight angulation. [8].
There is no established 'standard' treatment for buckle fractures but methods vary from soft bandages to removable splints to stricter immobilisation methods such as casting for 2-4 weeks, with regular follow-ups until fracture union [9], though there is growing evidence that plaster casts are unnecessary [10]. The need for follow-up is similarly uncertain, with around 50% of hospitals in the UK routinely planning no follow-up after this diagnosis in the ED (Emergency Department). [11] A national guideline from the UK National Institute for Clinical Excellence (NICE) identified that all treatments appeared safe and recommended either a removable splint or a bandage, without the need for a follow-up. In fact, the NICE guideline questioned whether any treatment was necessary at all for these fractures. [12] Studies have shown that, with removable methods at home, without the necessity of a follow-up appointment, parental satisfaction of nearly 100% is achieved. [13]
Given the ongoing variation in treatment, in terms of type of immobilisation, and necessity for follow-up, the National Institute for Health Research in the UK [14] have funded a randomised controlled trial, to definitively address this uncertainty. The trial, led by the University of Oxford, is called the FORCE study [15] and is a large pragmatic trial underway at 23 ED's, throughout the UK. [16] The trial is expected to report in Summer 2021.
- ^ Naranje, S. M., Erali, R. A., Warner, W. C., Sawyer, J. R., & Kelly, D. M. (2016). Epidemiology of Pediatric Fractures Presenting to Emergency Departments in the United States. Journal of Pediatric Orthopaedics, 36(4), e45–e48. doi:10.1097
- ^ Della-Giustina, D.A., Della-Giustina, K., 1999. Orthopaedic injuries: emergency department evaluation and treatment of pediatric orthopaedic injuries. Emergency Medicine Clinics of North America 17 (4)
- ^ Sharp, J. W., & Edwards, R. M. (2017). Core curriculum illustration: pediatric buckle fracture of the distal radius. Emergency Radiology. doi:10.1007
- ^ Wheeless, C.R., 2007. Wheeless Textbook of Orthopaedics. Duke Orthopaedics, North Carolina.
- ^ Randsborg P, Sivertsen E (2009) Distal radius fractures in children: substantial difference in stability between buckle and greenstick fractures. Acta Orthop 80(5):585–589. doi:10.3109/ 17453670903316850
- ^ van Bosse, H.J.P., Patel, R.J., Thacker, M., Sala, D.A., 2005. Minimalistic approach to treating wrist torus fractures. Journal of Orthopaedics 25 (4), 495–500.
- ^ Firmin, F., & Crouch, R. (2009). Splinting versus casting of “torus” fractures to the distal radius in the paediatric patient presenting at the emergency department (ED): A literature review. International Emergency Nursing, 17(3), 173–178. doi:10.1016
- ^ Eiff, M.P., Hatch, R.L., 2003. Boning up on common pediatric fractures. Contemporary Pediatrics 20.
- ^ Wilkins K, Upper Extremity. In: Rockwood C, Wilkins K, Beaty J, editors. Fractures in Children. 4th ed. New York: Raven, 1996 p. 483
- ^ Hill, Christopher & Masters, James & Perry, Daniel. (2015). A systematic review of alternative splinting versus complete plaster casts for the management of childhood buckle fractures of the wrist. Journal of pediatric orthopedics. Part B. 25. 10.1097
- ^ Widnall, J., Capstick, T., Wijesekera, M., Messahel, S. and Perry, D., 2020. Pain scores in torus fractures. Bone & Joint Open, [online] 1(2), pp.3-7. Available at: <https://online.boneandjoint.org.uk/doi/full/10.1302/2633-1462.12.BJO-2019-0002> [Accessed 21 December 2020].
- ^ Nice.org.uk. 2020. Overview | Fractures (Non-Complex): Assessment And Management | Guidance | NICE. [online] Available at: <https://www.nice.org.uk/guidance/ng38> [Accessed 21 December 2020].
- ^ Solan, M. ., Rees, R., & Daly, K. (2002). Current management of torus fractures of the distal radius. Injury, 33(6), 503–505. doi:10.1016
- ^ En.wikipedia.org. 2020. National Institute For Health Research. [online] Available at: </info/en/?search=National_Institute_for_Health_Research> [Accessed 21 December 2020].
- ^ Perry, D., 2020. FORCE Study. [online] Force.octru.ox.ac.uk. Available at: <https://force.octru.ox.ac.uk> [Accessed 21 December 2020].
- ^ Achten, J., Knight, R., Dutton, S., Costa, M., Mason, J., Dritsaki, M., Appelbe, D., Messahel, S., Roland, D., Widnall, J. and Perry, D., 2020. A multicentre prospective randomized equivalence trial of a soft bandage and immediate discharge versus current treatment with rigid immobilization for torus fractures of the distal radius in children. Bone & Joint Open, [online] 1(6), pp.214-221. Available at: <https://online.boneandjoint.org.uk/doi/full/10.1302/2633-1462.16.BJO-2020-0014.R1> [Accessed 21 December 2020].


Fractures of the wrist account for a third of all childhood fractures, with 1 in every 100 children presenting either a torus or a greenstick fracture.
Torus fractures are compression failures of the bone and are the most common fractures in children. [1] It is a common occurrence following a fall, as the wrist absorbs most of the impact and compresses the bony cortex on one side and remains intact on the other, creating a bulging effect. [2] For this reason, it is often referred to as an 'incomplete fracture' as the break is only on the one side. The compressive force is provided by the trabeculae and is longitudinal to the axis of the long bone [3]. The word "torus" originates from the Latin word "protuberance." [4]
Torus fractures are low risk and may cause acute pain. As the bone buckles (or crushes), instead of breaking, they are a stable injury as there is no displacement of the bone. [5] This mechanism is analogous to the crumple zones in cars. As with other fractures, the site of fracture may be tender to touch and cause a sharp pain if pressure is exerted on the injured area.
Physical activities or sports such as bike riding or climbing increase the associated risk for buckle fractures in the potential event of a collision or fall. As aforementioned, the most common buckle fracture is of the distal radius in the forearm, which typically originates from a Fall Onto an Outstretched Hand ( FOOSH) [6]. Such orthopaedic injuries are distinctive in children as their bones are softer and in a dynamic state of bone growth and development, with a higher collagen to bone ratio so incomplete fractures such as the buckle fracture are a more common occurrence. [7]
Buckle fracturs can be identified by performing a radiograph. The diagnosis of a torus fracture is made from both anterior/posterior and lateral projections. The typical features include:
- The buckling of cortical bone, which may appear as a small bulge or protuberance in the radius or ulna.
- The bone may have a slight angulation. [8].
There is no established 'standard' treatment for buckle fractures but methods vary from soft bandages to removable splints to stricter immobilisation methods such as casting for 2-4 weeks, with regular follow-ups until fracture union [9], though there is growing evidence that plaster casts are unnecessary [10]. The need for follow-up is similarly uncertain, with around 50% of hospitals in the UK routinely planning no follow-up after this diagnosis in the ED (Emergency Department). [11] A national guideline from the UK National Institute for Clinical Excellence (NICE) identified that all treatments appeared safe and recommended either a removable splint or a bandage, without the need for a follow-up. In fact, the NICE guideline questioned whether any treatment was necessary at all for these fractures. [12] Studies have shown that, with removable methods at home, without the necessity of a follow-up appointment, parental satisfaction of nearly 100% is achieved. [13]
Given the ongoing variation in treatment, in terms of type of immobilisation, and necessity for follow-up, the National Institute for Health Research in the UK [14] have funded a randomised controlled trial, to definitively address this uncertainty. The trial, led by the University of Oxford, is called the FORCE study [15] and is a large pragmatic trial underway at 23 ED's, throughout the UK. [16] The trial is expected to report in Summer 2021.
- ^ Naranje, S. M., Erali, R. A., Warner, W. C., Sawyer, J. R., & Kelly, D. M. (2016). Epidemiology of Pediatric Fractures Presenting to Emergency Departments in the United States. Journal of Pediatric Orthopaedics, 36(4), e45–e48. doi:10.1097
- ^ Della-Giustina, D.A., Della-Giustina, K., 1999. Orthopaedic injuries: emergency department evaluation and treatment of pediatric orthopaedic injuries. Emergency Medicine Clinics of North America 17 (4)
- ^ Sharp, J. W., & Edwards, R. M. (2017). Core curriculum illustration: pediatric buckle fracture of the distal radius. Emergency Radiology. doi:10.1007
- ^ Wheeless, C.R., 2007. Wheeless Textbook of Orthopaedics. Duke Orthopaedics, North Carolina.
- ^ Randsborg P, Sivertsen E (2009) Distal radius fractures in children: substantial difference in stability between buckle and greenstick fractures. Acta Orthop 80(5):585–589. doi:10.3109/ 17453670903316850
- ^ van Bosse, H.J.P., Patel, R.J., Thacker, M., Sala, D.A., 2005. Minimalistic approach to treating wrist torus fractures. Journal of Orthopaedics 25 (4), 495–500.
- ^ Firmin, F., & Crouch, R. (2009). Splinting versus casting of “torus” fractures to the distal radius in the paediatric patient presenting at the emergency department (ED): A literature review. International Emergency Nursing, 17(3), 173–178. doi:10.1016
- ^ Eiff, M.P., Hatch, R.L., 2003. Boning up on common pediatric fractures. Contemporary Pediatrics 20.
- ^ Wilkins K, Upper Extremity. In: Rockwood C, Wilkins K, Beaty J, editors. Fractures in Children. 4th ed. New York: Raven, 1996 p. 483
- ^ Hill, Christopher & Masters, James & Perry, Daniel. (2015). A systematic review of alternative splinting versus complete plaster casts for the management of childhood buckle fractures of the wrist. Journal of pediatric orthopedics. Part B. 25. 10.1097
- ^ Widnall, J., Capstick, T., Wijesekera, M., Messahel, S. and Perry, D., 2020. Pain scores in torus fractures. Bone & Joint Open, [online] 1(2), pp.3-7. Available at: <https://online.boneandjoint.org.uk/doi/full/10.1302/2633-1462.12.BJO-2019-0002> [Accessed 21 December 2020].
- ^ Nice.org.uk. 2020. Overview | Fractures (Non-Complex): Assessment And Management | Guidance | NICE. [online] Available at: <https://www.nice.org.uk/guidance/ng38> [Accessed 21 December 2020].
- ^ Solan, M. ., Rees, R., & Daly, K. (2002). Current management of torus fractures of the distal radius. Injury, 33(6), 503–505. doi:10.1016
- ^ En.wikipedia.org. 2020. National Institute For Health Research. [online] Available at: </info/en/?search=National_Institute_for_Health_Research> [Accessed 21 December 2020].
- ^ Perry, D., 2020. FORCE Study. [online] Force.octru.ox.ac.uk. Available at: <https://force.octru.ox.ac.uk> [Accessed 21 December 2020].
- ^ Achten, J., Knight, R., Dutton, S., Costa, M., Mason, J., Dritsaki, M., Appelbe, D., Messahel, S., Roland, D., Widnall, J. and Perry, D., 2020. A multicentre prospective randomized equivalence trial of a soft bandage and immediate discharge versus current treatment with rigid immobilization for torus fractures of the distal radius in children. Bone & Joint Open, [online] 1(6), pp.214-221. Available at: <https://online.boneandjoint.org.uk/doi/full/10.1302/2633-1462.16.BJO-2020-0014.R1> [Accessed 21 December 2020].