| Sjögren–Larsson syndrome | |
|---|---|
| Other names | SLS |
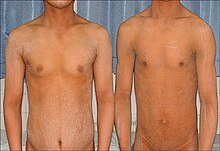 | |
| Two brothers (21 and 25 years old) with generalized dryness of skin with fine scales mainly around the umbilicus and in the flexural folds, one of Sjögren–Larsson syndrome characteristics. | |
| Specialty |
Medical genetics
|
Sjögren–Larsson syndrome is a rare autosomal recessive form of ichthyosis with neurological symptoms. [1]: 485 [2]: 564 [3] It can be identified by a triad of medical disorders. The first is ichthyosis, which is a buildup of skin to form a scale-like covering that causes dry skin and other problems. The second identifier is paraplegia which is characterized by leg spasms. The final identifier is intellectual delay.
SLS is caused by a mutation in the fatty aldehyde dehydrogenase gene found on chromosome 17. [4] In order for a child to receive SLS both parents must be carriers of the SLS gene. If they are carriers their child has a 1⁄4 chance of getting the disease. In 1957 SjГ¶gren and Larsson proposed that the Swedes with the disease all descended from a common ancestor 600 years ago. Today only 30–40 persons in Sweden have this disease. [5]
Signs and symptoms

- Dry and scaly skin similar to all other ichtyosiforms (types of ichthyosis).
- Neurological problems – this can often cause mild paralysis in the legs
- Mild to moderate intellectual disability.
- Often associated ocular features, which include pigmentary changes in the retina.
The usual presentation of crystalline maculopathy is from the age of 1–2 years onwards.[ citation needed]
Causes
It is associated with a deficiency of the enzyme fatty aldehyde dehydrogenase ( ALDH3A2) which is encoded on the short arm of chromosome 17 (17p11.2). At least 11 distinct mutations have been identified. [6]
Without a functioning fatty aldehyde dehydrogenase enzyme, the body is unable to break down medium- and long-chain fatty aldehydes which then build up in the membranes of the skin and brain. [4]
This condition is inherited in an autosomal recessive pattern. [7]
Diagnosis
Diagnosis is made with a blood test which sees if the activity of the fatty aldehyde dehydrogenase enzyme is normal. [4] Gene sequencing can also be used, which can additionally be used by would-be parents to see if they are carriers. [4]
Treatment
The ichthyosis is usually treated with topical ointment. [4] Anti-convulsants are used to treat seizures [4] and the spasms may be improved with surgery. [4]
Eponym
It was characterized by Torsten Sjögren and Tage Konrad Leopold Larsson (1905–1998), a Swedish medical statistician. [8] [9] It should not be confused with Sjögren's syndrome, which is a distinct condition named after a different person, Henrik Sjögren.[ citation needed]
See also
References
- ^ Freedberg, et al. (2003). Fitzpatrick's Dermatology in General Medicine. (6th ed.). McGraw-Hill. ISBN 0-07-138076-0.
- ^ James, William; Berger, Timothy; Elston, Dirk (2005). Andrews' Diseases of the Skin: Clinical Dermatology. (10th ed.). Saunders. ISBN 0-7216-2921-0.
- ^ Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. ISBN 978-1-4160-2999-1.
- ^ a b c d e f g "Sjogren-Larsson syndrome | Genetic and Rare Diseases Information Center (GARD) – an NCATS Program". rarediseases.info.nih.gov. Archived from the original on 2021-03-18. Retrieved 2020-10-31.
- ^ "Sjögren-Larssons syndrom". Archived from the original on 2018-01-23. Retrieved 2015-09-11.
- ^ Sillén A, Anton-Lamprecht I, Braun-Quentin C, et al. (1998). "Spectrum of mutations and sequence variants in the FALDH gene in patients with Sjögren–Larsson syndrome". Hum. Mutat. 12 (6): 377–84. doi: 10.1002/(SICI)1098-1004(1998)12:6<377::AID-HUMU3>3.0.CO;2-I. PMID 9829906. S2CID 37451614.
- ^ Orphanet: Portal de enfermedades raras y medicamentos huГ©rfanos
- ^ synd/1678 at Who Named It?
- ^ SJOGREN T, LARSSON T (1957). "Oligophrenia in combination with congenital ichthyosis and spastic disorders; a clinical and genetic study". Acta Psychiatr Neurol Scand Suppl. 113: 1–112. PMID 13457946.
Further reading
- Sjögren, K. G. Torsten; Larsson, Tage K. (1957). "Oligophrenia in combination with congenital ichtyosis and spastic disorders; a clinical and genetic study". Acta Psychiatrica Scandinavica. 32 (supplement 113). Copenhagen: 9–105. doi: 10.1111/j.1600-0447.1956.tb04725.x. PMID 13457946. S2CID 72058188.
External links
| Sjögren–Larsson syndrome | |
|---|---|
| Other names | SLS |
 | |
| Two brothers (21 and 25 years old) with generalized dryness of skin with fine scales mainly around the umbilicus and in the flexural folds, one of Sjögren–Larsson syndrome characteristics. | |
| Specialty |
Medical genetics
|
Sjögren–Larsson syndrome is a rare autosomal recessive form of ichthyosis with neurological symptoms. [1]: 485 [2]: 564 [3] It can be identified by a triad of medical disorders. The first is ichthyosis, which is a buildup of skin to form a scale-like covering that causes dry skin and other problems. The second identifier is paraplegia which is characterized by leg spasms. The final identifier is intellectual delay.
SLS is caused by a mutation in the fatty aldehyde dehydrogenase gene found on chromosome 17. [4] In order for a child to receive SLS both parents must be carriers of the SLS gene. If they are carriers their child has a 1⁄4 chance of getting the disease. In 1957 SjГ¶gren and Larsson proposed that the Swedes with the disease all descended from a common ancestor 600 years ago. Today only 30–40 persons in Sweden have this disease. [5]
Signs and symptoms

- Dry and scaly skin similar to all other ichtyosiforms (types of ichthyosis).
- Neurological problems – this can often cause mild paralysis in the legs
- Mild to moderate intellectual disability.
- Often associated ocular features, which include pigmentary changes in the retina.
The usual presentation of crystalline maculopathy is from the age of 1–2 years onwards.[ citation needed]
Causes
It is associated with a deficiency of the enzyme fatty aldehyde dehydrogenase ( ALDH3A2) which is encoded on the short arm of chromosome 17 (17p11.2). At least 11 distinct mutations have been identified. [6]
Without a functioning fatty aldehyde dehydrogenase enzyme, the body is unable to break down medium- and long-chain fatty aldehydes which then build up in the membranes of the skin and brain. [4]
This condition is inherited in an autosomal recessive pattern. [7]
Diagnosis
Diagnosis is made with a blood test which sees if the activity of the fatty aldehyde dehydrogenase enzyme is normal. [4] Gene sequencing can also be used, which can additionally be used by would-be parents to see if they are carriers. [4]
Treatment
The ichthyosis is usually treated with topical ointment. [4] Anti-convulsants are used to treat seizures [4] and the spasms may be improved with surgery. [4]
Eponym
It was characterized by Torsten Sjögren and Tage Konrad Leopold Larsson (1905–1998), a Swedish medical statistician. [8] [9] It should not be confused with Sjögren's syndrome, which is a distinct condition named after a different person, Henrik Sjögren.[ citation needed]
See also
References
- ^ Freedberg, et al. (2003). Fitzpatrick's Dermatology in General Medicine. (6th ed.). McGraw-Hill. ISBN 0-07-138076-0.
- ^ James, William; Berger, Timothy; Elston, Dirk (2005). Andrews' Diseases of the Skin: Clinical Dermatology. (10th ed.). Saunders. ISBN 0-7216-2921-0.
- ^ Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. ISBN 978-1-4160-2999-1.
- ^ a b c d e f g "Sjogren-Larsson syndrome | Genetic and Rare Diseases Information Center (GARD) – an NCATS Program". rarediseases.info.nih.gov. Archived from the original on 2021-03-18. Retrieved 2020-10-31.
- ^ "Sjögren-Larssons syndrom". Archived from the original on 2018-01-23. Retrieved 2015-09-11.
- ^ Sillén A, Anton-Lamprecht I, Braun-Quentin C, et al. (1998). "Spectrum of mutations and sequence variants in the FALDH gene in patients with Sjögren–Larsson syndrome". Hum. Mutat. 12 (6): 377–84. doi: 10.1002/(SICI)1098-1004(1998)12:6<377::AID-HUMU3>3.0.CO;2-I. PMID 9829906. S2CID 37451614.
- ^ Orphanet: Portal de enfermedades raras y medicamentos huГ©rfanos
- ^ synd/1678 at Who Named It?
- ^ SJOGREN T, LARSSON T (1957). "Oligophrenia in combination with congenital ichthyosis and spastic disorders; a clinical and genetic study". Acta Psychiatr Neurol Scand Suppl. 113: 1–112. PMID 13457946.
Further reading
- Sjögren, K. G. Torsten; Larsson, Tage K. (1957). "Oligophrenia in combination with congenital ichtyosis and spastic disorders; a clinical and genetic study". Acta Psychiatrica Scandinavica. 32 (supplement 113). Copenhagen: 9–105. doi: 10.1111/j.1600-0447.1956.tb04725.x. PMID 13457946. S2CID 72058188.