| Cold injury | |
|---|---|
| Other names | Cold weather injury |
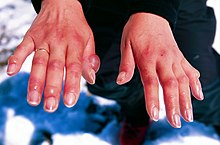 | |
| Frostbitten fingers after descent from mountain climbing | |
| Symptoms | Numbness, skin discoloration, blisters, swelling, cold sensation [1] [2] |
| Complications | Necrosis, gangrene, chronic pain, amputation [3] [4] |
| Types | Freezing, nonfreezing [5] |
| Causes | Exposure to cold temperatures [6] |
| Risk factors | Military occupation, recreational winter activities, homelessness, inadequate or wet clothing, substance abuse, diabetes, peripheral vascular disease [6] [7] |
| Diagnostic method | Based on symptoms [1] [6] |
| Differential diagnosis | Hypothermia, Raynaud's phenomenon, chilblains (pernio), cold urticaria [8] [9] |
| Prevention | Minimize cold exposure, wear protective clothing, change wet clothing, avoid substance use, maintain appropriate nutrition [1] [4] |
| Treatment | Move to warm and dry environment, rewarming, medication, wound care, surgery [4] [10] |
Cold injury (or cold weather injury) is damage to the body from cold exposure, including hypothermia and several skin injuries. [6] Cold-related skin injuries are categorized into freezing and nonfreezing cold injuries. [5] Freezing cold injuries involve tissue damage when exposed to temperatures below freezing (less than 0 degrees Celsius). [6] [7] Nonfreezing cold injuries involve tissue damage when exposed to temperatures often between 0-15 degrees Celsius for extended periods of time. [6] While these injuries have disproportionally affected military members, recreational winter activities have also increased the risk and incidence within civilian populations. [6] Additional risk factors include homelessness, inadequate or wet clothing, alcohol abuse or tobacco abuse, and pre-existing medical conditions that impair blood flow. [6] [7]
Freezing cold skin injuries include frostbite and frostnip. [8] These injuries often affect the fingers, toes, nose, and ears since they are less commonly covered by clothing when in cold environments. [1] Affected skin becomes numb, turns white or blue, and develops blisters. [1] Frostnip is a superficial skin injury that won't freeze the skin or cause long-term damage. [8] Frostbite involves freezing of fluids inside and outside of cells that results in cell breakdown, electrolyte imbalances, and inflammation. [8] Surrounding blood vessel constriction and injury disrupts blood flow to affected tissue, which may cause tissue death ( necrosis). [11] Diagnosis is based on symptoms, but imaging can help assess viable tissue and risk of amputation. [6] Pre-hospital treatment involves transfer to a warm environment, changing wet clothing, and rapid rewarming with warm water if refreezing is not expected. [11] Hospital management involves rewarming, wound care, and medications to treat pain and possible blood clots. [11] Amputation of unsalvageable tissue may be required weeks to months after initial injury. [11]
Nonfreezing cold skin injuries include trench foot, a subclass of immersion foot caused by exposure to cold temperatures. [2] These injuries often affect the feet after being subjected to wet cold for several hours or days. [4] Affected individuals report a tingling or numbing sensation, red or blue discoloration, and swelling or blisters in affected skin. [2] The mechanism of injury isn't fully understood, but may involve cold-induced damage to blood vessels and nerves that results in small blood vessel ( capillary) destruction, swelling, and tissue necrosis. [5] Diagnosis is based on symptoms. [2] Pre-hospital treatment includes transfer to a warm environment and exchanging wet clothing. [4] Hospital management includes gradual rewarming with air drying, elevating affected skin, and pain management. [4]
There is lacking comprehensive data on the overall incidence of freezing cold injuries, including frostbite. [3] Military populations have been disproportionally affected due to prolonged cold exposure associated with work requirements. [6] From 2015-2020, the United States military reported 1,120 frostbite cases. [8] Increased incidence of cases have been noted in individuals who participate in winter recreational activities, especially mountaineering. [3]
Several physical, behavioral, and environmental risk factors contribute to freezing cold injury cases. These include homelessness, inadequate clothing, high altitude, dehydration, and alcohol or tobacco abuse. [6] [7] Individuals with previous cold injury are at increased risk for another cold injury. [7] Pre-existing medical conditions that compromise blood flow, such as diabetes, Raynaud syndrome, and peripheral vascular disease increase risk of injury. [7] [3]
Damage from freezing cold injury occurs through direct freezing of tissue, disrupted blood flow to affected skin, and rewarming injury. [8] [11] [3] Freezing causes ice crystal formation in tissue that disrupts cell membranes and surrounding blood vessels. [11] Electrolyte imbalances, tissue swelling ( edema), and inflammation occur as intracellular contents enter surrounding tissue fluid. [11] Constriction of blood vessels in response to freezing can cause tissue death (necrosis) in severe cases due to blood vessel blockage. [11]
During the rewarming process, restored blood flow induces further inflammatory damage via formation of reactive oxygen species. [7] [3] This inflammation involves specific molecules ( prostaglandins, thromboxanes, bradykinin, histamine) that cause edema and damage to blood vessels, leading to potential blood clot formation and interruption of blood flow. [3]
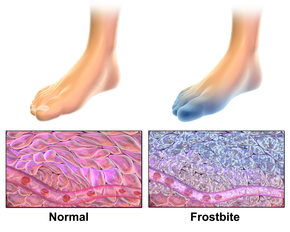
Freezing cold injuries are diagnosed based on symptom presentation, but several weeks are often needed to determine the full extent of tissue injury. [6] In suspected severe cases, magnetic resonance angiography (MRA) or Technetium-99 bone scan may be used after injury to determine the likelihood of tissue recovery and potential need for amputation. [6] [1] Bone scanning can help determine the ability to use tissue plasminogen activator (tPA) for breaking up associated blood clots. [1]
In cases of suspected freezing cold injury, other cold-induced conditions should be evaluated and treated appropriately. [6] These conditions may include:
Hypothermia: An accidental reduction of core body temperature to less than 35 degrees Celsius, most commonly due to cold environment exposure. [9] Often presents as uncontrollable shivering that may progress to impaired consciousness and abnormal vital signs. [9] Severe cases can cause cardiac arrest. [9] Hypothermia should be treated first, if present, by bringing core body temperature above 35 degrees Celsius. [6] [10]
Raynaud's phenomenon: An abnormal spasming of blood vessels often in the tips of fingers and toes - usually in response to strong emotions or cold exposure. [8] The digits will turn a white or blue color. [8] This can be a primary disorder or secondary to an underlying medical condition. [8]
Affected individuals should be moved to a warm environment and have wet clothing removed and replaced. [10] Rewarming should only be attempted when there is no risk of refreezing, as this would worsen tissue damage. [11] [10] Rewarming should not involve rubbing or massaging affected skin to avoid worsening the injury. [10] Placing affected skin in an armpit, groin crease, or warm water bath are viable rewarming options. [11] [10] Aloe vera gel and NSAIDs can help reduce inflammation. [11]
Choice of rewarming method depends on the suspected extent of skin injury and severity of hypothermia (if present). [11] Passive rewarming techniques such as blankets may be sufficient for milder injuries. [11] Active rewarming techniques such as warm intravenous fluids or warm water baths may be needed for more severe injuries. [11] [10] Rewarming should be continued until affected skin becomes red or purple in color and softens. [10] Pain management with NSAIDs or opioids should be provided. [10]
Topical Aloe vera gel should be applied to thawed tissue prior to dressing application. [10] Clear or cloudy blisters may be drained with needle aspiration, but hemorrhagic blisters should be left intact. [10] Consider antibiotics for severe injuries with potential tissue necrosis or gangrene. [10] Tetanus toxoid should be administered based on local guidelines. [10]
Using tissue plasminogen activator (tPA) within 24 hours of injury can both reduce tissue damage and increase amount of salvageable tissue by breaking up blood clots. [11] This has led to a corresponding reduction of amputations in previous trials. [11] Iloprost may be used to dilate blood vessels and decrease platelet aggregation when tPA is contraindicated or ineffective. [11] [10] Reducing clotting ability with streptokinase or heparin can reduce the risk of amputation. [10]
Surgical treatment may include removal of dead/damaged tissue ( debridement) or amputation and is usually performed several weeks after initial injury. [11] [10] Urgent surgery is needed when sepsis, severe infection, or wet gangrene is present. [10] Fasciotomy may be required if compartment syndrome develops in the affected limb. [11] [10]
Recommended preventative measures for freezing cold injuries include appropriate nutrition, wearing suitable clothing that covers one's skin, avoiding constrictive clothing, and ensuring access to warm shelter. [1] [11] Alcohol and other substance use should be discouraged. [1]

Long-term complications of freezing cold injury depend on the extent of tissue damage. [1] Higher degrees of injury with firm skin after rewarming, hemorrhagic blisters, and tissue necrosis or gangrene carry a worse prognosis. [1] In addition to possible amputation, several complications have been reported months or years after initial injury . [3] These include chronic pain, increased sensitivity to cold, abnormal skin sensation, and arthritis. [3] Long-term impaired circulation of blood flow and nerve damage have been attributed as possible causes. [3]
Freezing cold injury on the hands and feet can be graded to estimate risk of amputation. [1]
Grade 1: absence of bluish discoloration of skin ( cyanosis); no risk of amputation or long-term complications
Grade 2: cyanosis on distal phalanges; possible amputation of fingertip/tip of toe and fingernail/toenail
Grade 3: cyanosis on intermediate and proximal phalanges; possible amputation to bone of digit with functional impairment
Grade 4: cyanosis over the carpal/ tarsal bones; possible amputation to limb with functional impairment
Nonfreezing cold injuries occur in individuals with cold, wet skin for prolonged periods of time (several hours to days). [4] These injuries have been characterized in military populations, who may be unable to frequently change their environmental surroundings or wet clothing. [8] [4] However, civilian populations with occupations that expose them to cold standing water, such as hikers, [15] or that participate in winter recreational activities are also at risk. [4] Additional risk factors include immobility, homelessness, alcohol or tobacco abuse, elderly age, dehydration, and underlying medical conditions such as peripheral vascular disease and diabetes. [6] [7]
The underlying mechanism of nonfreezing cold injury isn't fully understood, but has been characterized by poor blood flow into tissue exposed to cold, wet conditions. [15] This may result in destruction of small blood vessels, which leads to swelling, nerve damage, and tissue breakdown due to pressure injury. [5] [15]
Distinction between acute and chronic mechanisms of nonfreezing cold injury has been discussed. [5] Acute cases involve disruption of blood flow with breakdown of affected tissue and nerve damage. [5] Chronic cases can occur after multiple episodes of acute injury, with partial restoration of blood flow but persistence of long-term symptoms. [5]

Nonfreezing cold injury commonly affects the feet due to prolonged exposure to wet socks or cold standing water. [4] Symptoms progress through a series of four stages. [4] [15]

During cold exposure
- Affected skin becomes numb, which can cause a clumsy walking pattern ( gait) if the feet are affected
- Skin transitions from red to a pale color depending on temperature of exposure [4] [15]
After cold exposure
- Symptoms can last from a few hours to a few days
- During rewarming, skin appears pale blue and continue to be cold, numb, and swollen [4] [15]
Increased blood flow to affected tissue ( hyperemia)
- Symptoms can last from a few days to several weeks
- Affected limb becomes red and swollen with bounding pulses
- Numbness is replaced with increased sensitivity to pain
- Severely damaged tissue may develop blisters due to pressure injury or infection [4] [15]
After hyperemia
- Symptoms can last from a few weeks to several years
- Skin changes resolve (unless necrosis has occurred), but injured limb remains sensitive to cold [4] [15]
Nonfreezing cold injury is diagnosed based on symptoms and history of prolonged exposure (usually 12 hours to 4 days) to cold moisture above freezing temperatures. [7] Those affected report loss of sensation in affected skin for at least 30 minutes and abnormal sensation when experiencing rewarming. [4] The use of imaging or lab testing specific to nonfreezing cold injury is not helpful for confirming the diagnosis. [4] Imaging may be indicated to work up possible trauma or infection. [4]
Other related cold-induced conditions include:
Chilblains (pernio): Inflammatory skin injury that can be caused by exposure to nonfreezing cold. [8] Presents as red patches and plaques that resolve after a few weeks. [8] Chronic cases have been reported in individuals with repeated cold exposure. [8] Pernio-like skin lesions have also been associated with previous SARS-CoV-2 infection. [8]
Cold urticaria: An allergic reaction that occurs when skin is exposed to cold stimuli. [8] [4] Lesions resemble hives ( urticaria). [4] This condition can occur secondary to certain infections and medications. [8]
Individuals with suspected nonfreezing cold injury should be moved to a warm, dry environment and have wet clothing swapped with dry replacements. [4] Rewarming should be done gradually at room temperature with affected skin exposed to air and elevated above heart level. [4] In contrast, rapid rewarming has been associated with worsening pain and tissue injury. [4] Affected skin should not be rubbed or massaged to avoid further damage. [4] Intravenous fluids should be warmed prior to infusion to reduce further heat loss. [4]
Pain management should be achieved with amitriptyline, as NSAIDs and opioids are not as effective. [4] Use of gabapentin and medications to dilate blood vessels ( vasodilators) for pain control remains controversial. [6] [4]

Antibiotics usually aren't necessary, but should be started if infectious complications such as fungal infection or cellulitis occurs. [5] [4] If necrotic tissue is present, surgical debridement or amputation may be necessary. [5]
Recommended preventative measures include minimizing skin contact with wet cold, keeping clothing warm and dry, and elevating one's feet. [4] Cotton clothing should be avoided in cold, wet environments as it retains moisture easily. [4] In outdoor occupations, rotating personnel minimizes risk of prolonged cold exposure. [4]
Most cases of nonfreezing cold injury resolve with minimal tissue loss, but some cases can be complicated by infection, nail loss, excess sweating ( hyperhidrosis), and chronic pain or abnormal sensations in the affected skin. [7] [4] Injury to blood vessels and nerves in the affected skin with persistent constriction of blood vessels causes most long-term complications. [4] Chronic pain is associated with increased risk of mental health conditions, including depression, suicidal ideation, and alcohol abuse. [4]

Cold injuries have occurred for millennia, with the first documented case discovered in a 5000 year-old mummy within the Chilean mountains. [6] The first mass instance of cold injury was notably documented by Baron Larrey during Napoleon's retreat from Russia in the winter of 1812-1813. [10] These injuries also plagued thousands of soldiers during World War I and II. [5] [8] Trench foot is thought to have contributed up to 75,000 deaths among British soldiers during World War I, with the condition obtaining its name from its association with trench warfare. [5] [8] Over 25,000 cases of trench foot were reported among US military during World War II. [8] Preventative measures such as rotating trench positions, changing socks multiple times per day, and using whale oil on one's feet were introduced to reduce incidence of cases. [2] Cold skin injuries are still prominent in the modern era, with 1,120 cases of frostbite and 590 cases of trench foot reported in the US military from 2015-2020. [8]
- ^ a b c d e f g h i j k l Basit, Hajira; Wallen, Tanner J.; Dudley, Christopher (2022), "Frostbite", StatPearls, Treasure Island (FL): StatPearls Publishing, PMID 30725599, retrieved 2022-11-09
- ^ a b c d e Bush, Jeffrey S.; Lofgran, Trevor; Watson, Simon (2022), "Trench Foot", StatPearls, Treasure Island (FL): StatPearls Publishing, PMID 29493986, retrieved 2022-11-09
- ^ a b c d e f g h i j Regli, Ivo B.; Strapazzon, Giacomo; Falla, Marika; Oberhammer, Rosmarie; Brugger, Hermann (2021). "Long-Term Sequelae of Frostbite—A Scoping Review". International Journal of Environmental Research and Public Health. 18 (18): 9655. doi: 10.3390/ijerph18189655. ISSN 1660-4601. PMC 8465633. PMID 34574580.
- ^ a b c d e f g h i j k l m n o p q r s t u v w x y z aa ab ac ad ae af ag ah Zafren, Ken (2021). "Nonfreezing Cold Injury (Trench Foot)". International Journal of Environmental Research and Public Health. 18 (19): 10482. doi: 10.3390/ijerph181910482. ISSN 1660-4601. PMC 8508462. PMID 34639782.
- ^ a b c d e f g h i j k Mistry, K.; Ondhia, C.; Levell, N. J. (2020). "A review of trench foot: a disease of the past in the present". Clinical and Experimental Dermatology. 45 (1): 10–14. doi: 10.1111/ced.14031. ISSN 0307-6938. PMID 31309614. S2CID 196810788.
- ^ a b c d e f g h i j k l m n o p q r Heil, Kieran; Thomas, Rachel; Robertson, Greg; Porter, Anna; Milner, Robert; Wood, Alexander (2016). "Freezing and non-freezing cold weather injuries: a systematic review". British Medical Bulletin. 117 (1): 79–93. doi: 10.1093/bmb/ldw001. ISSN 0007-1420. PMID 26872856.
- ^ a b c d e f g h i j Ingram, Benjamin J.; Raymond, Tyler J. (2013). "Recognition and Treatment of Freezing and Nonfreezing Cold Injuries". Current Sports Medicine Reports. 12 (2): 125–130. doi: 10.1249/JSR.0b013e3182877454. ISSN 1537-890X. PMID 23478565. S2CID 39830023.
- ^ a b c d e f g h i j k l m n o p q r s t Kowtoniuk, Robert (2021-10-01). "Cutaneous Cold Weather Injuries in the US Military". Cutis. 108 (4): 181–184. doi: 10.12788/cutis.0363. PMID 34846996. S2CID 243974698.
- ^ a b c d Paal, Peter; Pasquier, Mathieu; Darocha, Tomasz; Lechner, Raimund; Kosinski, Sylweriusz; Wallner, Bernd; Zafren, Ken; Brugger, Hermann (2022-01-03). "Accidental Hypothermia: 2021 Update". International Journal of Environmental Research and Public Health. 19 (1): 501. doi: 10.3390/ijerph19010501. ISSN 1660-4601. PMC 8744717. PMID 35010760.
- ^ a b c d e f g h i j k l m n o p q r s Handford, Charles; Buxton, Pauline; Russell, Katie; Imray, Caitlin EA; McIntosh, Scott E.; Freer, Luanne; Cochran, Amalia; Imray, Christopher HE (2014-04-22). "Frostbite: a practical approach to hospital management". Extreme Physiology & Medicine. 3 (1): 7. doi: 10.1186/2046-7648-3-7. ISSN 2046-7648. PMC 3994495. PMID 24764516.
- ^ a b c d e f g h i j k l m n o p q r s t Joshi, Kumud; Goyary, Danswrang; Mazumder, Bhaskar; Chattopadhyay, Pronobesh; Chakraborty, Reshmi; Bhutia, Y. D.; Karmakar, Sanjeev; Dwivedi, Sanjai Kumar (2020-10-01). "Frostbite: Current status and advancements in therapeutics". Journal of Thermal Biology. 93: 102716. doi: 10.1016/j.jtherbio.2020.102716. ISSN 0306-4565. PMID 33077129. S2CID 224810280.
- ^ McIntosh, Scott E.; Opacic, Matthew; Freer, Luanne; Grissom, Colin K.; Auerbach, Paul S.; Rodway, George W.; Cochran, Amalia; Giesbrecht, Gordon G.; McDevitt, Marion (1 December 2014). "Wilderness Medical Society practice guidelines for the prevention and treatment of frostbite: 2014 update". Wilderness & Environmental Medicine. 25 (4 Suppl): S43–54. doi: 10.1016/j.wem.2014.09.001. ISSN 1545-1534. PMID 25498262.
- ^ "Frostbite Clinical Presentation". emedicine.medscape.com. Archived from the original on 2 March 2017. Retrieved 2 March 2017.
- ^ Zafren, Ken (2013). "Frostbite: Prevention and Initial Management". High Altitude Medicine & Biology. 14 (1): 9–12. doi: 10.1089/ham.2012.1114. PMID 23537254. S2CID 3036889.
- ^ a b c d e f g h Zafren, Ken; Danzl, Daniel; Ganetsky, Michael (2022). "Nonfreezing cold water (trench foot) and warm water immersion injuries". UpToDate.
| Cold injury | |
|---|---|
| Other names | Cold weather injury |
 | |
| Frostbitten fingers after descent from mountain climbing | |
| Symptoms | Numbness, skin discoloration, blisters, swelling, cold sensation [1] [2] |
| Complications | Necrosis, gangrene, chronic pain, amputation [3] [4] |
| Types | Freezing, nonfreezing [5] |
| Causes | Exposure to cold temperatures [6] |
| Risk factors | Military occupation, recreational winter activities, homelessness, inadequate or wet clothing, substance abuse, diabetes, peripheral vascular disease [6] [7] |
| Diagnostic method | Based on symptoms [1] [6] |
| Differential diagnosis | Hypothermia, Raynaud's phenomenon, chilblains (pernio), cold urticaria [8] [9] |
| Prevention | Minimize cold exposure, wear protective clothing, change wet clothing, avoid substance use, maintain appropriate nutrition [1] [4] |
| Treatment | Move to warm and dry environment, rewarming, medication, wound care, surgery [4] [10] |
Cold injury (or cold weather injury) is damage to the body from cold exposure, including hypothermia and several skin injuries. [6] Cold-related skin injuries are categorized into freezing and nonfreezing cold injuries. [5] Freezing cold injuries involve tissue damage when exposed to temperatures below freezing (less than 0 degrees Celsius). [6] [7] Nonfreezing cold injuries involve tissue damage when exposed to temperatures often between 0-15 degrees Celsius for extended periods of time. [6] While these injuries have disproportionally affected military members, recreational winter activities have also increased the risk and incidence within civilian populations. [6] Additional risk factors include homelessness, inadequate or wet clothing, alcohol abuse or tobacco abuse, and pre-existing medical conditions that impair blood flow. [6] [7]
Freezing cold skin injuries include frostbite and frostnip. [8] These injuries often affect the fingers, toes, nose, and ears since they are less commonly covered by clothing when in cold environments. [1] Affected skin becomes numb, turns white or blue, and develops blisters. [1] Frostnip is a superficial skin injury that won't freeze the skin or cause long-term damage. [8] Frostbite involves freezing of fluids inside and outside of cells that results in cell breakdown, electrolyte imbalances, and inflammation. [8] Surrounding blood vessel constriction and injury disrupts blood flow to affected tissue, which may cause tissue death ( necrosis). [11] Diagnosis is based on symptoms, but imaging can help assess viable tissue and risk of amputation. [6] Pre-hospital treatment involves transfer to a warm environment, changing wet clothing, and rapid rewarming with warm water if refreezing is not expected. [11] Hospital management involves rewarming, wound care, and medications to treat pain and possible blood clots. [11] Amputation of unsalvageable tissue may be required weeks to months after initial injury. [11]
Nonfreezing cold skin injuries include trench foot, a subclass of immersion foot caused by exposure to cold temperatures. [2] These injuries often affect the feet after being subjected to wet cold for several hours or days. [4] Affected individuals report a tingling or numbing sensation, red or blue discoloration, and swelling or blisters in affected skin. [2] The mechanism of injury isn't fully understood, but may involve cold-induced damage to blood vessels and nerves that results in small blood vessel ( capillary) destruction, swelling, and tissue necrosis. [5] Diagnosis is based on symptoms. [2] Pre-hospital treatment includes transfer to a warm environment and exchanging wet clothing. [4] Hospital management includes gradual rewarming with air drying, elevating affected skin, and pain management. [4]
There is lacking comprehensive data on the overall incidence of freezing cold injuries, including frostbite. [3] Military populations have been disproportionally affected due to prolonged cold exposure associated with work requirements. [6] From 2015-2020, the United States military reported 1,120 frostbite cases. [8] Increased incidence of cases have been noted in individuals who participate in winter recreational activities, especially mountaineering. [3]
Several physical, behavioral, and environmental risk factors contribute to freezing cold injury cases. These include homelessness, inadequate clothing, high altitude, dehydration, and alcohol or tobacco abuse. [6] [7] Individuals with previous cold injury are at increased risk for another cold injury. [7] Pre-existing medical conditions that compromise blood flow, such as diabetes, Raynaud syndrome, and peripheral vascular disease increase risk of injury. [7] [3]
Damage from freezing cold injury occurs through direct freezing of tissue, disrupted blood flow to affected skin, and rewarming injury. [8] [11] [3] Freezing causes ice crystal formation in tissue that disrupts cell membranes and surrounding blood vessels. [11] Electrolyte imbalances, tissue swelling ( edema), and inflammation occur as intracellular contents enter surrounding tissue fluid. [11] Constriction of blood vessels in response to freezing can cause tissue death (necrosis) in severe cases due to blood vessel blockage. [11]
During the rewarming process, restored blood flow induces further inflammatory damage via formation of reactive oxygen species. [7] [3] This inflammation involves specific molecules ( prostaglandins, thromboxanes, bradykinin, histamine) that cause edema and damage to blood vessels, leading to potential blood clot formation and interruption of blood flow. [3]

Freezing cold injuries are diagnosed based on symptom presentation, but several weeks are often needed to determine the full extent of tissue injury. [6] In suspected severe cases, magnetic resonance angiography (MRA) or Technetium-99 bone scan may be used after injury to determine the likelihood of tissue recovery and potential need for amputation. [6] [1] Bone scanning can help determine the ability to use tissue plasminogen activator (tPA) for breaking up associated blood clots. [1]
In cases of suspected freezing cold injury, other cold-induced conditions should be evaluated and treated appropriately. [6] These conditions may include:
Hypothermia: An accidental reduction of core body temperature to less than 35 degrees Celsius, most commonly due to cold environment exposure. [9] Often presents as uncontrollable shivering that may progress to impaired consciousness and abnormal vital signs. [9] Severe cases can cause cardiac arrest. [9] Hypothermia should be treated first, if present, by bringing core body temperature above 35 degrees Celsius. [6] [10]
Raynaud's phenomenon: An abnormal spasming of blood vessels often in the tips of fingers and toes - usually in response to strong emotions or cold exposure. [8] The digits will turn a white or blue color. [8] This can be a primary disorder or secondary to an underlying medical condition. [8]
Affected individuals should be moved to a warm environment and have wet clothing removed and replaced. [10] Rewarming should only be attempted when there is no risk of refreezing, as this would worsen tissue damage. [11] [10] Rewarming should not involve rubbing or massaging affected skin to avoid worsening the injury. [10] Placing affected skin in an armpit, groin crease, or warm water bath are viable rewarming options. [11] [10] Aloe vera gel and NSAIDs can help reduce inflammation. [11]
Choice of rewarming method depends on the suspected extent of skin injury and severity of hypothermia (if present). [11] Passive rewarming techniques such as blankets may be sufficient for milder injuries. [11] Active rewarming techniques such as warm intravenous fluids or warm water baths may be needed for more severe injuries. [11] [10] Rewarming should be continued until affected skin becomes red or purple in color and softens. [10] Pain management with NSAIDs or opioids should be provided. [10]
Topical Aloe vera gel should be applied to thawed tissue prior to dressing application. [10] Clear or cloudy blisters may be drained with needle aspiration, but hemorrhagic blisters should be left intact. [10] Consider antibiotics for severe injuries with potential tissue necrosis or gangrene. [10] Tetanus toxoid should be administered based on local guidelines. [10]
Using tissue plasminogen activator (tPA) within 24 hours of injury can both reduce tissue damage and increase amount of salvageable tissue by breaking up blood clots. [11] This has led to a corresponding reduction of amputations in previous trials. [11] Iloprost may be used to dilate blood vessels and decrease platelet aggregation when tPA is contraindicated or ineffective. [11] [10] Reducing clotting ability with streptokinase or heparin can reduce the risk of amputation. [10]
Surgical treatment may include removal of dead/damaged tissue ( debridement) or amputation and is usually performed several weeks after initial injury. [11] [10] Urgent surgery is needed when sepsis, severe infection, or wet gangrene is present. [10] Fasciotomy may be required if compartment syndrome develops in the affected limb. [11] [10]
Recommended preventative measures for freezing cold injuries include appropriate nutrition, wearing suitable clothing that covers one's skin, avoiding constrictive clothing, and ensuring access to warm shelter. [1] [11] Alcohol and other substance use should be discouraged. [1]

Long-term complications of freezing cold injury depend on the extent of tissue damage. [1] Higher degrees of injury with firm skin after rewarming, hemorrhagic blisters, and tissue necrosis or gangrene carry a worse prognosis. [1] In addition to possible amputation, several complications have been reported months or years after initial injury . [3] These include chronic pain, increased sensitivity to cold, abnormal skin sensation, and arthritis. [3] Long-term impaired circulation of blood flow and nerve damage have been attributed as possible causes. [3]
Freezing cold injury on the hands and feet can be graded to estimate risk of amputation. [1]
Grade 1: absence of bluish discoloration of skin ( cyanosis); no risk of amputation or long-term complications
Grade 2: cyanosis on distal phalanges; possible amputation of fingertip/tip of toe and fingernail/toenail
Grade 3: cyanosis on intermediate and proximal phalanges; possible amputation to bone of digit with functional impairment
Grade 4: cyanosis over the carpal/ tarsal bones; possible amputation to limb with functional impairment
Nonfreezing cold injuries occur in individuals with cold, wet skin for prolonged periods of time (several hours to days). [4] These injuries have been characterized in military populations, who may be unable to frequently change their environmental surroundings or wet clothing. [8] [4] However, civilian populations with occupations that expose them to cold standing water, such as hikers, [15] or that participate in winter recreational activities are also at risk. [4] Additional risk factors include immobility, homelessness, alcohol or tobacco abuse, elderly age, dehydration, and underlying medical conditions such as peripheral vascular disease and diabetes. [6] [7]
The underlying mechanism of nonfreezing cold injury isn't fully understood, but has been characterized by poor blood flow into tissue exposed to cold, wet conditions. [15] This may result in destruction of small blood vessels, which leads to swelling, nerve damage, and tissue breakdown due to pressure injury. [5] [15]
Distinction between acute and chronic mechanisms of nonfreezing cold injury has been discussed. [5] Acute cases involve disruption of blood flow with breakdown of affected tissue and nerve damage. [5] Chronic cases can occur after multiple episodes of acute injury, with partial restoration of blood flow but persistence of long-term symptoms. [5]

Nonfreezing cold injury commonly affects the feet due to prolonged exposure to wet socks or cold standing water. [4] Symptoms progress through a series of four stages. [4] [15]

During cold exposure
- Affected skin becomes numb, which can cause a clumsy walking pattern ( gait) if the feet are affected
- Skin transitions from red to a pale color depending on temperature of exposure [4] [15]
After cold exposure
- Symptoms can last from a few hours to a few days
- During rewarming, skin appears pale blue and continue to be cold, numb, and swollen [4] [15]
Increased blood flow to affected tissue ( hyperemia)
- Symptoms can last from a few days to several weeks
- Affected limb becomes red and swollen with bounding pulses
- Numbness is replaced with increased sensitivity to pain
- Severely damaged tissue may develop blisters due to pressure injury or infection [4] [15]
After hyperemia
- Symptoms can last from a few weeks to several years
- Skin changes resolve (unless necrosis has occurred), but injured limb remains sensitive to cold [4] [15]
Nonfreezing cold injury is diagnosed based on symptoms and history of prolonged exposure (usually 12 hours to 4 days) to cold moisture above freezing temperatures. [7] Those affected report loss of sensation in affected skin for at least 30 minutes and abnormal sensation when experiencing rewarming. [4] The use of imaging or lab testing specific to nonfreezing cold injury is not helpful for confirming the diagnosis. [4] Imaging may be indicated to work up possible trauma or infection. [4]
Other related cold-induced conditions include:
Chilblains (pernio): Inflammatory skin injury that can be caused by exposure to nonfreezing cold. [8] Presents as red patches and plaques that resolve after a few weeks. [8] Chronic cases have been reported in individuals with repeated cold exposure. [8] Pernio-like skin lesions have also been associated with previous SARS-CoV-2 infection. [8]
Cold urticaria: An allergic reaction that occurs when skin is exposed to cold stimuli. [8] [4] Lesions resemble hives ( urticaria). [4] This condition can occur secondary to certain infections and medications. [8]
Individuals with suspected nonfreezing cold injury should be moved to a warm, dry environment and have wet clothing swapped with dry replacements. [4] Rewarming should be done gradually at room temperature with affected skin exposed to air and elevated above heart level. [4] In contrast, rapid rewarming has been associated with worsening pain and tissue injury. [4] Affected skin should not be rubbed or massaged to avoid further damage. [4] Intravenous fluids should be warmed prior to infusion to reduce further heat loss. [4]
Pain management should be achieved with amitriptyline, as NSAIDs and opioids are not as effective. [4] Use of gabapentin and medications to dilate blood vessels ( vasodilators) for pain control remains controversial. [6] [4]

Antibiotics usually aren't necessary, but should be started if infectious complications such as fungal infection or cellulitis occurs. [5] [4] If necrotic tissue is present, surgical debridement or amputation may be necessary. [5]
Recommended preventative measures include minimizing skin contact with wet cold, keeping clothing warm and dry, and elevating one's feet. [4] Cotton clothing should be avoided in cold, wet environments as it retains moisture easily. [4] In outdoor occupations, rotating personnel minimizes risk of prolonged cold exposure. [4]
Most cases of nonfreezing cold injury resolve with minimal tissue loss, but some cases can be complicated by infection, nail loss, excess sweating ( hyperhidrosis), and chronic pain or abnormal sensations in the affected skin. [7] [4] Injury to blood vessels and nerves in the affected skin with persistent constriction of blood vessels causes most long-term complications. [4] Chronic pain is associated with increased risk of mental health conditions, including depression, suicidal ideation, and alcohol abuse. [4]

Cold injuries have occurred for millennia, with the first documented case discovered in a 5000 year-old mummy within the Chilean mountains. [6] The first mass instance of cold injury was notably documented by Baron Larrey during Napoleon's retreat from Russia in the winter of 1812-1813. [10] These injuries also plagued thousands of soldiers during World War I and II. [5] [8] Trench foot is thought to have contributed up to 75,000 deaths among British soldiers during World War I, with the condition obtaining its name from its association with trench warfare. [5] [8] Over 25,000 cases of trench foot were reported among US military during World War II. [8] Preventative measures such as rotating trench positions, changing socks multiple times per day, and using whale oil on one's feet were introduced to reduce incidence of cases. [2] Cold skin injuries are still prominent in the modern era, with 1,120 cases of frostbite and 590 cases of trench foot reported in the US military from 2015-2020. [8]
- ^ a b c d e f g h i j k l Basit, Hajira; Wallen, Tanner J.; Dudley, Christopher (2022), "Frostbite", StatPearls, Treasure Island (FL): StatPearls Publishing, PMID 30725599, retrieved 2022-11-09
- ^ a b c d e Bush, Jeffrey S.; Lofgran, Trevor; Watson, Simon (2022), "Trench Foot", StatPearls, Treasure Island (FL): StatPearls Publishing, PMID 29493986, retrieved 2022-11-09
- ^ a b c d e f g h i j Regli, Ivo B.; Strapazzon, Giacomo; Falla, Marika; Oberhammer, Rosmarie; Brugger, Hermann (2021). "Long-Term Sequelae of Frostbite—A Scoping Review". International Journal of Environmental Research and Public Health. 18 (18): 9655. doi: 10.3390/ijerph18189655. ISSN 1660-4601. PMC 8465633. PMID 34574580.
- ^ a b c d e f g h i j k l m n o p q r s t u v w x y z aa ab ac ad ae af ag ah Zafren, Ken (2021). "Nonfreezing Cold Injury (Trench Foot)". International Journal of Environmental Research and Public Health. 18 (19): 10482. doi: 10.3390/ijerph181910482. ISSN 1660-4601. PMC 8508462. PMID 34639782.
- ^ a b c d e f g h i j k Mistry, K.; Ondhia, C.; Levell, N. J. (2020). "A review of trench foot: a disease of the past in the present". Clinical and Experimental Dermatology. 45 (1): 10–14. doi: 10.1111/ced.14031. ISSN 0307-6938. PMID 31309614. S2CID 196810788.
- ^ a b c d e f g h i j k l m n o p q r Heil, Kieran; Thomas, Rachel; Robertson, Greg; Porter, Anna; Milner, Robert; Wood, Alexander (2016). "Freezing and non-freezing cold weather injuries: a systematic review". British Medical Bulletin. 117 (1): 79–93. doi: 10.1093/bmb/ldw001. ISSN 0007-1420. PMID 26872856.
- ^ a b c d e f g h i j Ingram, Benjamin J.; Raymond, Tyler J. (2013). "Recognition and Treatment of Freezing and Nonfreezing Cold Injuries". Current Sports Medicine Reports. 12 (2): 125–130. doi: 10.1249/JSR.0b013e3182877454. ISSN 1537-890X. PMID 23478565. S2CID 39830023.
- ^ a b c d e f g h i j k l m n o p q r s t Kowtoniuk, Robert (2021-10-01). "Cutaneous Cold Weather Injuries in the US Military". Cutis. 108 (4): 181–184. doi: 10.12788/cutis.0363. PMID 34846996. S2CID 243974698.
- ^ a b c d Paal, Peter; Pasquier, Mathieu; Darocha, Tomasz; Lechner, Raimund; Kosinski, Sylweriusz; Wallner, Bernd; Zafren, Ken; Brugger, Hermann (2022-01-03). "Accidental Hypothermia: 2021 Update". International Journal of Environmental Research and Public Health. 19 (1): 501. doi: 10.3390/ijerph19010501. ISSN 1660-4601. PMC 8744717. PMID 35010760.
- ^ a b c d e f g h i j k l m n o p q r s Handford, Charles; Buxton, Pauline; Russell, Katie; Imray, Caitlin EA; McIntosh, Scott E.; Freer, Luanne; Cochran, Amalia; Imray, Christopher HE (2014-04-22). "Frostbite: a practical approach to hospital management". Extreme Physiology & Medicine. 3 (1): 7. doi: 10.1186/2046-7648-3-7. ISSN 2046-7648. PMC 3994495. PMID 24764516.
- ^ a b c d e f g h i j k l m n o p q r s t Joshi, Kumud; Goyary, Danswrang; Mazumder, Bhaskar; Chattopadhyay, Pronobesh; Chakraborty, Reshmi; Bhutia, Y. D.; Karmakar, Sanjeev; Dwivedi, Sanjai Kumar (2020-10-01). "Frostbite: Current status and advancements in therapeutics". Journal of Thermal Biology. 93: 102716. doi: 10.1016/j.jtherbio.2020.102716. ISSN 0306-4565. PMID 33077129. S2CID 224810280.
- ^ McIntosh, Scott E.; Opacic, Matthew; Freer, Luanne; Grissom, Colin K.; Auerbach, Paul S.; Rodway, George W.; Cochran, Amalia; Giesbrecht, Gordon G.; McDevitt, Marion (1 December 2014). "Wilderness Medical Society practice guidelines for the prevention and treatment of frostbite: 2014 update". Wilderness & Environmental Medicine. 25 (4 Suppl): S43–54. doi: 10.1016/j.wem.2014.09.001. ISSN 1545-1534. PMID 25498262.
- ^ "Frostbite Clinical Presentation". emedicine.medscape.com. Archived from the original on 2 March 2017. Retrieved 2 March 2017.
- ^ Zafren, Ken (2013). "Frostbite: Prevention and Initial Management". High Altitude Medicine & Biology. 14 (1): 9–12. doi: 10.1089/ham.2012.1114. PMID 23537254. S2CID 3036889.
- ^ a b c d e f g h Zafren, Ken; Danzl, Daniel; Ganetsky, Michael (2022). "Nonfreezing cold water (trench foot) and warm water immersion injuries". UpToDate.